Cardiac Catheterizations
What Is a Cardiac Catheterization?
A cardiac catheterization is a procedure in which a catheter, or a long hollow tube, is inserted through an artery towards the heart. Dye is then injected under x-ray in order to visualize the arteries of the heart muscle. If necessary, a stent may be inserted in order to open a blocked artery.
Traditionally a heart catheterization procedure is performed through an artery in the groin. However, the interventional cardiologists of Hunterdon Cardiovascular Associates, under the lead of William Schafranek, MD, Medical Director of the Cardiac Catheterization laboratory at Hunterdon Medical Center, are trained at completing this procedure through an artery in the wrist.This is known as the transradial approach and is a technique that enhances patient comfort as well as mobility after the procedure. In addition, the transradial approach provides patients with a significantly shorter hospital stay. At the same time, this approach reduces the risk of bleeding complications. With close to 85% of our cardiac catheterizations done transradially, far exceeding the national average, our interventional cardiologists are among the most experienced in the state at this technique.
Our interventional cardiologists also offer, and are proficient at, using some of the most cutting-edge technology currently available for the interventional treatment of coronary artery disease, including bioabsorbable stents, calcium cutting tools, and the Impella percutaneous left ventricular assist device.
How Does Cardiac Catheterization Differ From Peripheral Catheterization?
Peripheral catheterization involves opening up blocked arteries in the peripheral vasculature, including the extremities, the gut, and the kidneys, while cardiac catheterization focuses only on the arteries of the heart. Peripheral catheterization can be used to treat deep venous thrombosis of the extremities as well. The interventional cardiologists of HCA combine this with a guideline-based approach for noninvasive screening in partnership with our accredited vascular imaging department. We treat patients with both acute and chronic symptoms of peripheral artery disease.
Am I a Candidate for a Cardiac Catheterization?
Your doctor may request a heart catheterization if you experience any of the following:
- Dramatically abnormal stress test results
- Heart failure that may be associated with coronary artery disease
- Angina that disrupts daily living and is difficult to control with medication
- Symptoms of heart valve disease, such as shortness of breath
- Unidentifiable recurrent chest pain
What to Expect When Getting a Cardiac or Peripheral Vascular Catheterization
How Is a Cardiac Catheterization Procedure Performed?
Cardiac catheterization takes place in an operating room equipped with special imaging devices. This may be referred to as a cardiac cath lab.
Typically, patients are sedated before their procedure begins, remaining awake but calm and comfortable. Your doctor will discuss your anesthesia with you prior to your procedure based on the particular details of your case.
- Before catheterization, an IV line is inserted into the arm. As arranged, additional medication may be administered through this IV during the procedure.
- Electrodes will be placed on the chest to monitor your heartbeat.
- The site where the catheter will be inserted may be shaved. An injection of numbing medication will be administered at this site.
- After the tissue has become numb, a small nick is made in the skin. A plastic sheath is inserted into this tiny incision, and the catheter is passed through.
Once the catheter has been inserted, a number of different processes may take place. Cardiac catheterization may facilitate:
- Coronary angiogram to check for arterial blockages
- Right heart catheterization to assess blood flow from the right side of the heart
- Balloon angioplasty with or without stenting to open a blocked artery
- Heart ablation to correct an irregular heartbeat
How To Prepare For Your Cardiac Catheterization
Your doctor may provide you with detailed instructions regarding preparation for your cardiac catheterization procedure, but generally, patients should do the following:
- Avoid blood-thinning medications in the days before cardiac catheterization (but not typically aspirin or other anti-platelet medications). A physician will discuss this with you before your procedure.
- Discuss exact dosages of medications currently taken. Patients may be asked to bring original bottles of all medications and supplements with them to their test.
- Avoid eating and drinking in the 6 hours before cardiac catheterization. Diabetic patients may need to discuss medication and insulin instructions with their doctor.
- Implement relaxation techniques to calm nerves before and during testing. Medication may be given before cardiac catheterization to help reduce anxiety.
What Is The Recovery From A Cardiac Catheterization Procedure?
Initial recovery takes place in a recovery area where our staff will monitor your vital signs while the anesthesia wears off. At this time, the plastic sheath that secured the catheter will be removed. After approximately one hour, once anesthesia has worn off, the patient is released to an outpatient room or hospital room if they will have an overnight stay. It may be necessary to lie flat on the back for several hours after the procedure. Patients can resume eating and drinking shortly after the test and some patients return home on the day of their procedure.
What Results Can I Expect From Cardiac Catheterization?
The results of cardiac catheterization can be used to diagnose coronary artery disease, heart valve disease, cardiomyopathy or congestive heart failure. The report will note the state of each coronary artery and its level of calcification or narrowing. The procedure can also be useful in treating heart problems. The report will include the findings as well as how the procedure was done, if there were any complications, and whether the procedure was successful.
Why Is a Cardiac Catheterization Important? A Patient Story
The patient is a 91 year old female admitted to the hospital with shortness of breath and chest pain. She denied any significant past cardiac history. A cardiac catheterization showed a severe blockage in the left main coronary artery and another blockage in the left circumflex.
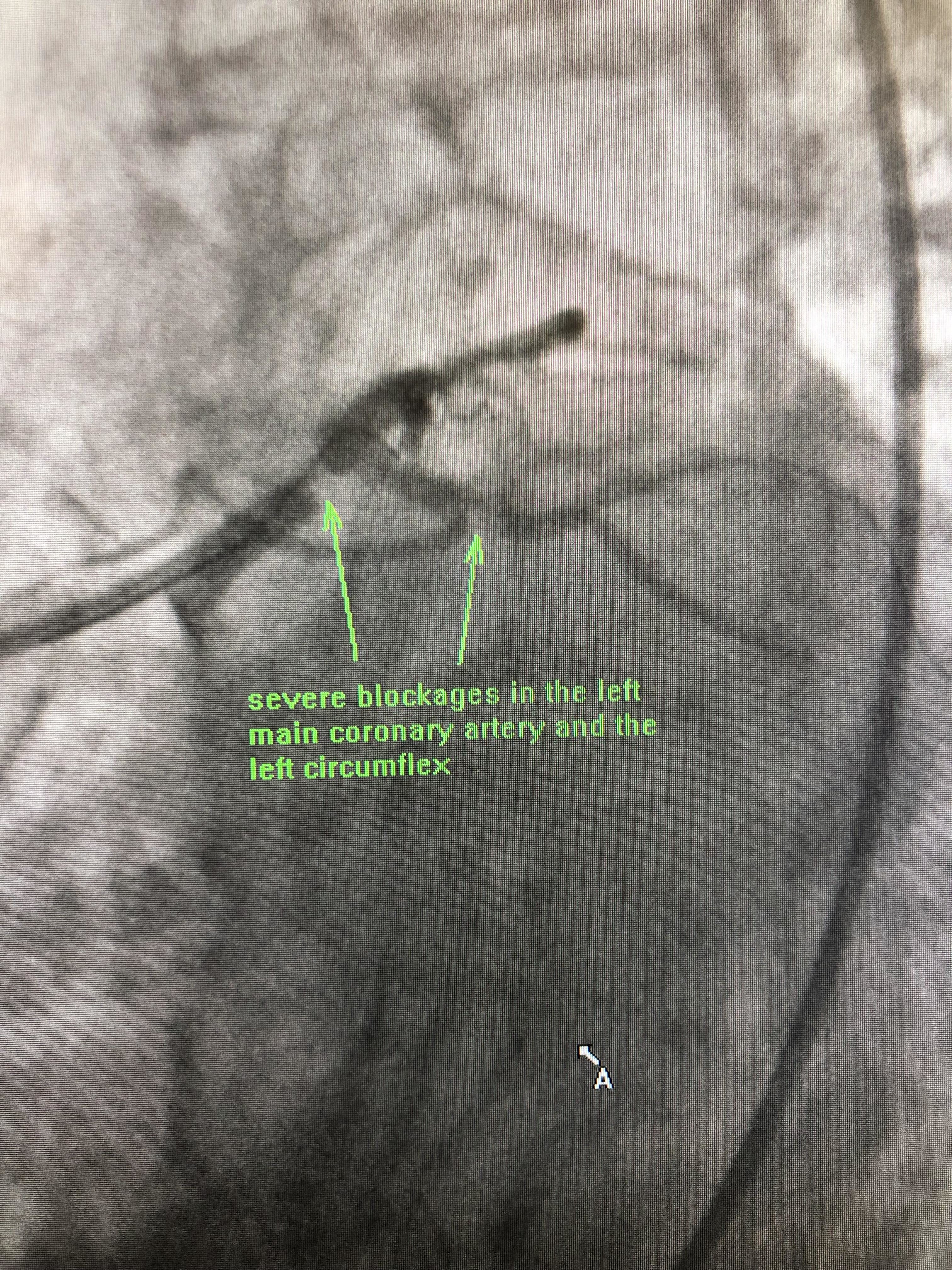
Blockages in the left main coronary artery are felt to be best treated with open heart surgery and she was referred to a surgeon for an evaluation. She was evaluated by cardiac surgery and because of her age and other non-cardiac medical history, she was considered a poor candidate for cardiac bypass surgery. She continued to have chest pain with minimal activity, and after discussion with her family, medical team, and Dr. Schafranek a decision was made to proceed with a high risk procedure to place a stent in the left main coronary artery.
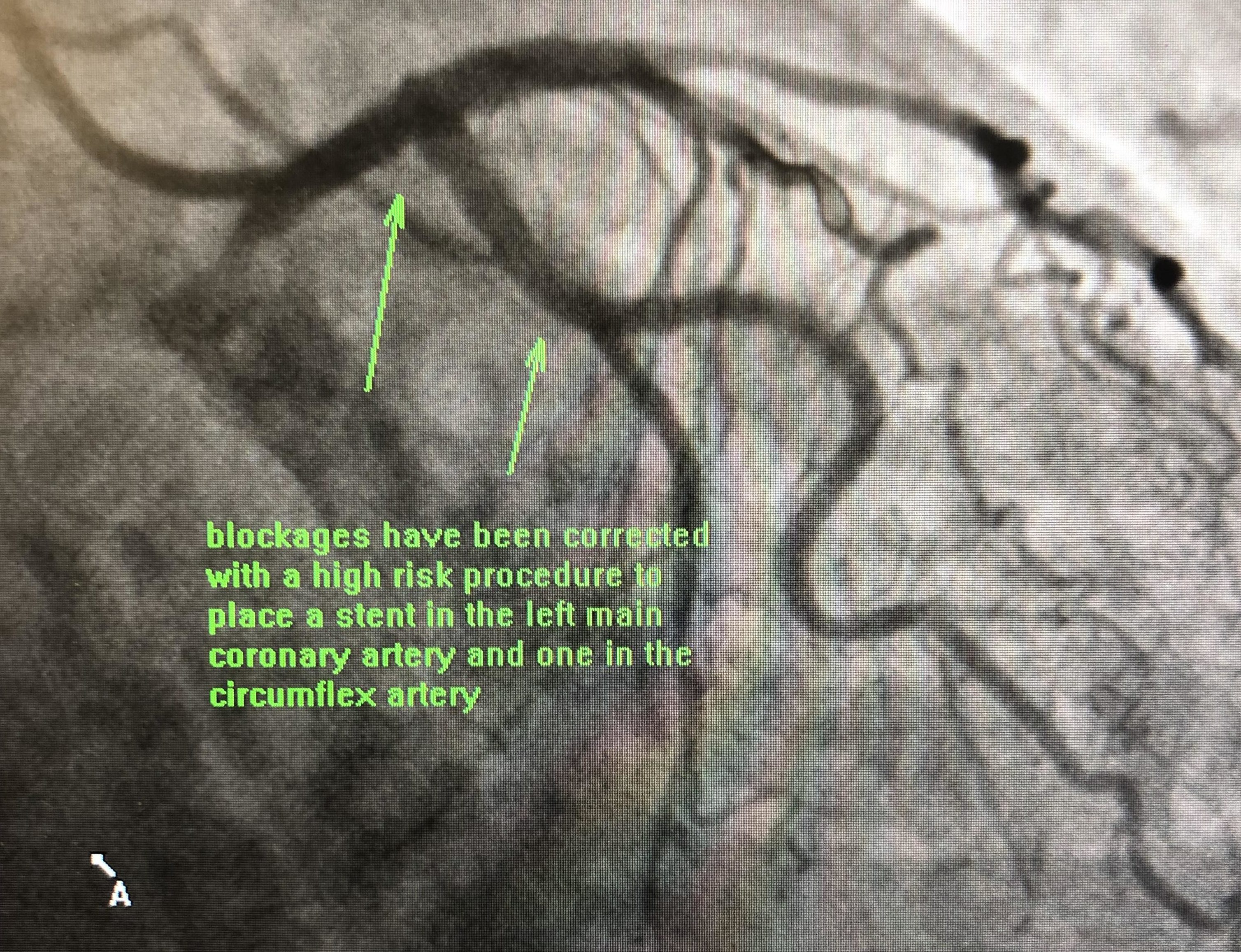
She underwent this procedure without any complications and was discharged the following day. She did very well after the procedure.
Schedule a Consultation
For more information on cardiac catheterization or to schedule an appointment, call (908) 788.1710. Visit one of our locations in Flemington, Bridgewater, and Clinton, New Jersey.


